Chronic joint pain is one of the most common and debilitating conditions affecting millions of people worldwide. Whether it’s caused by arthritis, injury or age-related wear and tear, persistent pain can significantly reduce mobility, disrupt sleep and impact overall quality of life. Many individuals try medications, physical therapy or steroid injections, only to find that relief is temporary or incomplete. If you are searching for a more effective and longer-lasting solution, Radiofrequency Ablation may be the answer.
Radiofrequency Ablation is a minimally invasive nerve ablation procedure designed to target and disrupt the nerves responsible for transmitting pain signals. Unlike treatments that simply mask symptoms, this advanced technique focuses on eliminating pain at its source. As a widely used method of RFA for pain, it has become a preferred option for patients suffering from chronic joint conditions, especially in the spine, knees and hips.
In this comprehensive guide, we will explore everything you need to know about Radiofrequency Ablation, including how it works, the different types available, its benefits, potential risks and what you can expect before, during and after the procedure. By the end of this article, you will have a clear understanding of how this innovative nerve ablation procedure can provide long-term relief and help you regain control of your daily life.
What Is Radiofrequency Ablation?
Understanding Radiofrequency Ablation in Detail
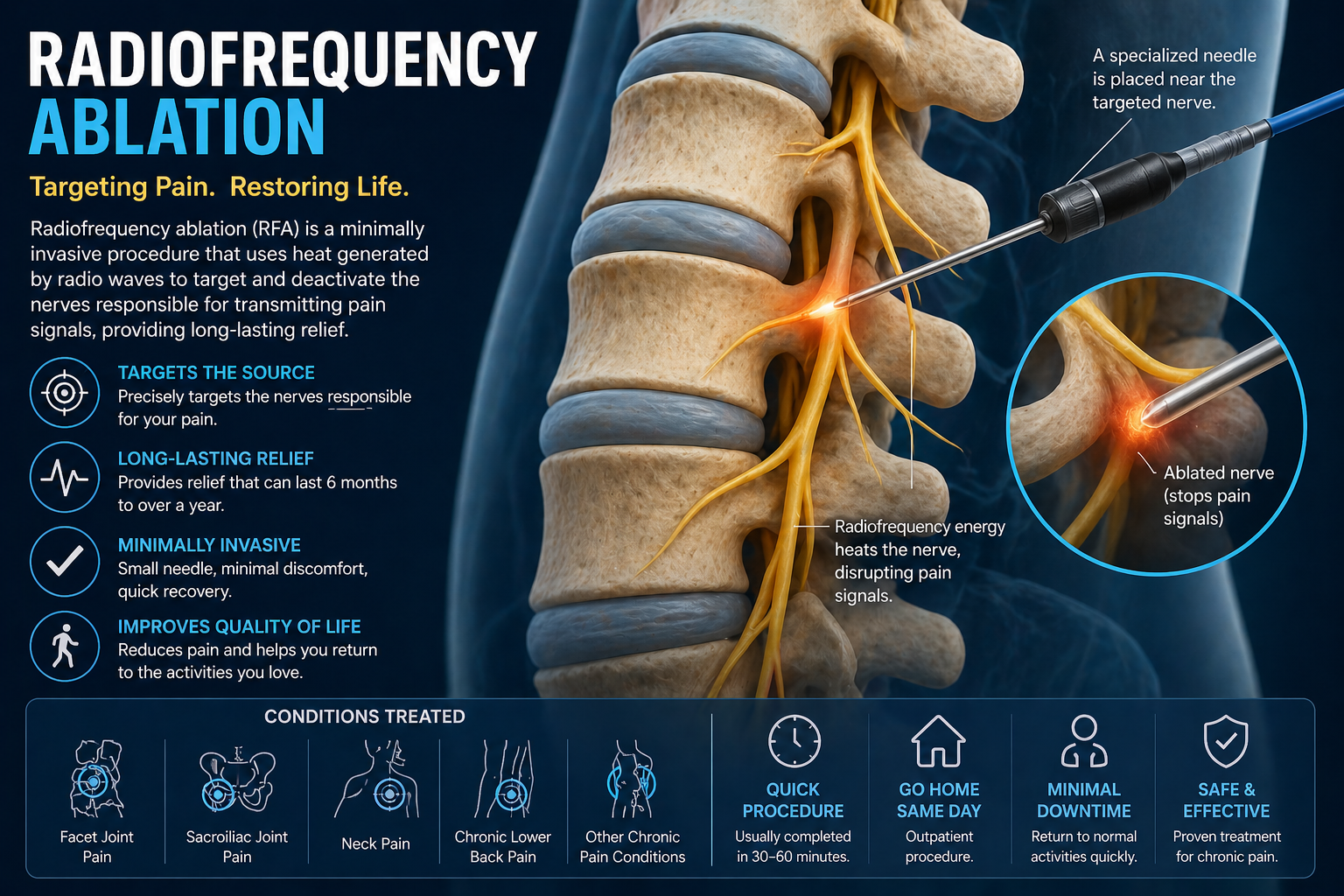
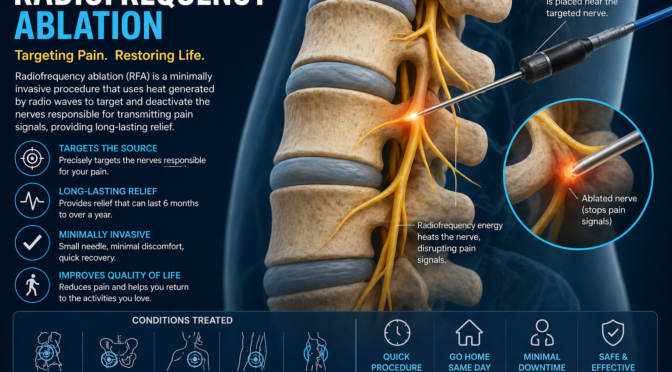
Radiofrequency Ablation is a specialized medical technique used to treat chronic pain by targeting specific nerves and disrupting their ability to transmit pain signals. This procedure uses heat generated by radiofrequency energy to create a controlled lesion on the nerve, effectively reducing its function.
Unlike surgical procedures, this nerve ablation procedure does not involve large incisions or removal of tissue. Instead, it is performed using a thin needle inserted through the skin, making it a minimally invasive option with a relatively quick recovery time. Patients who undergo RFA for pain often report significant improvement in their symptoms, especially when the source of pain has been accurately identified.
This treatment is commonly recommended for individuals who have already tried conservative therapies such as medications or physical therapy without achieving lasting relief. It is also frequently used after successful diagnostic nerve blocks, which help confirm the exact nerve responsible for the pain.
How Radiofrequency Ablation Works?
The effectiveness of Radiofrequency Ablation lies in its ability to interrupt the transmission of pain signals. Pain travels through nerves to the brain, where it is interpreted as discomfort. By applying controlled heat to these nerves, the procedure disrupts their ability to send signals.
During the nerve ablation procedure, a specialized needle is guided to the target nerve using imaging technology such as fluoroscopy. Once in position, radiofrequency energy is delivered through the needle, heating the nerve tissue and creating a lesion. This process reduces the nerve’s ability to function, thereby decreasing pain.
Key mechanisms include:
- Blocking pain signals before they reach the brain
- Reducing nerve sensitivity in the affected area
- Providing sustained relief for months or longer
This makes RFA for pain an effective solution for patients seeking long-term relief without relying on medications.
Conditions Treated with Radiofrequency Ablation
Radiofrequency Ablation is widely used to treat various chronic pain conditions, particularly those involving joints and the spine.
Common conditions include:
- Facet joint arthritis in the spine
- Chronic neck and lower back pain
- Knee osteoarthritis
- Hip joint pain
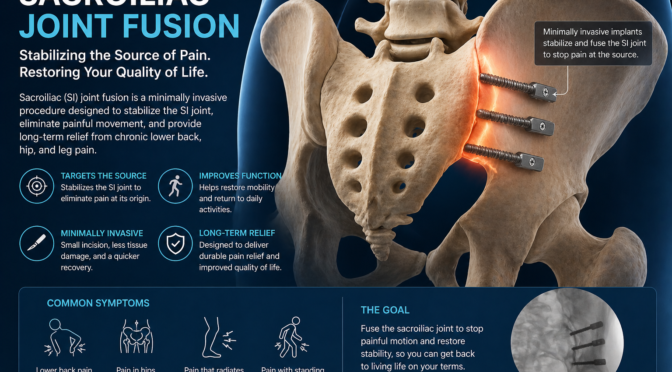
- Sacroiliac joint dysfunction
This versatile nerve ablation procedure is especially beneficial for patients whose pain originates from specific nerve pathways.
Types of Radiofrequency Ablation Procedures
Conventional Radiofrequency Ablation
Conventional Radiofrequency Ablation is the most performed technique. It uses continuous radiofrequency energy to generate heat and create a precise lesion on the targeted nerve.
This method of RFA for pain is highly effective for treating localized pain conditions, particularly those involving the spine. The precision of this technique ensures that only the targeted nerve is affected, minimizing the risk of damage to surrounding tissues.
Patients who undergo this type of nerve ablation procedure often experience significant pain relief that lasts for several months.
Pulsed Radiofrequency Ablation
Pulsed Radiofrequency Ablation is a variation that uses intermittent bursts of energy instead of continuous heat. This approach is less aggressive and is often used for sensitive nerves or areas where preserving nerve function is important.
Benefits include:
- Reduced risk of nerve damage
- Suitable for delicate or complex cases
- Provides pain modulation rather than complete nerve disruption
This form of RFA for pain is ideal for patients who require a more conservative approach to treatment.
Cooled Radiofrequency Ablation
Cooled Radiofrequency Ablation is an advanced technique that uses water-cooled electrodes to create larger and more uniform lesions. This allows for better coverage of the targeted nerve area, increasing the likelihood of successful pain relief.
Advantages include:
- Greater precision and effectiveness
- Ability to treat larger joints such as the knee
- Longer-lasting results
This modern nerve ablation procedure has become increasingly popular due to its enhanced outcomes and reliability.
Benefits of Radiofrequency Ablation
Long-Lasting Pain Relief
One of the key benefits of Radiofrequency Ablation is its ability to deliver long-lasting pain relief. Unlike temporary treatments such as injections, this nerve ablation procedure can reduce pain for several months or even up to a year.
Patients undergoing RFA for pain often report a substantial decrease in discomfort, allowing them to return to normal activities with greater ease.
Minimally Invasive and Quick Recovery
Radiofrequency Ablation is a minimally invasive procedure, meaning it does not require major surgery or extended hospital stays.
Key benefits include:
- Performed on an outpatient basis
- Minimal downtime
- Faster recovery compared to surgery
This makes the nerve ablation procedure an attractive option for patients seeking effective treatment without the risks of invasive surgery.
Reduced Dependence on Medications
Chronic pain is often managed with medications that can cause side effects or lead to dependency. Radiofrequency Ablation addresses the root cause of pain, reducing the need for ongoing medication use.
Benefits include:
- Lower risk of addiction
- Fewer side effects
- Improved overall health
This makes RFA for pain a safer and more sustainable solution for long-term pain management.
Procedure: What to Expect
Before the Procedure
Before undergoing Radiofrequency Ablation, patients undergo a thorough evaluation to ensure they are suitable candidates. This includes reviewing medical history, conducting imaging tests and performing diagnostic nerve blocks.
These steps help confirm the source of pain and increase the likelihood of success for the nerve ablation procedure.
During the Procedure
The procedure itself is relatively quick and typically takes between 30 and 60 minutes.
Steps include:
- Cleaning and numbing the treatment area
- Using imaging guidance to position the needle
- Delivering radiofrequency energy to the target nerve
Throughout the RFA for pain procedure, patients remain awake but comfortable.
After the Procedure
After Radiofrequency Ablation, patients are monitored briefly before being discharged.
Post-procedure care includes:
- Resting for 24 hours
- Avoiding strenuous activities
- Gradually resuming normal routines
Most patients notice pain relief within a few days to weeks.
Risks and Side Effects
Common Side Effects
While Radiofrequency Ablation is generally safe, some mild side effects may occur.
These include:
- Temporary soreness at the treatment site
- Mild swelling or bruising
- Slight numbness
Potential Risks
Although rare, complications can occur, including infection or nerve irritation.
Choosing an experienced provider reduces risks associated with this nerve ablation procedure.
How Are Risks Minimized?
Doctors use imaging guidance and sterile techniques to ensure the safety of RFA for pain procedures.
Is Radiofrequency Ablation Right for You?
Ideal Candidates
Radiofrequency Ablation is ideal for patients with chronic joint pain who have not responded to other treatments.
Consultation and Decision-Making
A thorough consultation helps determine whether this nerve ablation procedure is suitable for your condition.
Conclusion
Radiofrequency Ablation is a highly effective and minimally invasive solution for chronic joint pain. By targeting the nerves responsible for pain signals, this advanced nerve ablation procedure provides long-lasting relief and improves overall quality of life. As a proven method of RFA for pain, it offers a safe and reliable alternative to surgery and long-term medication use.
If you are ready to take the next step toward pain relief, book a consultation today and discover how Radiofrequency Ablation can help you regain mobility and live a more comfortable life.