What does modern healthcare require to enhance patient outcomes and support long-term satisfaction? Across the healthcare industry providers are increasingly recognizing that successful treatment involves more than simply addressing symptoms. Patients want personalized communication accessible care and treatment plans designed around their individual needs. This growing shift has fuelled the rise of patient-centered care USA initiatives across hospitals clinics and specialty practices.
This transformation is being driven in part by healthcare leaders such as Dr. Rodolfo Gari. With decades of experience in medicine pain management and healthcare operations Dr. Gari has helped develop care models focused on improving the patient experience while supporting clinical excellence. His work as a physician entrepreneur and healthcare executive has focused on broadening access to specialized treatment and strengthening physician-patient relationships.
His work reflects many of the principles shaping modern healthcare including personalized treatment plans integrated services and improved access to specialty care. Through leadership in pain management organizations and healthcare practice development he has helped support broader conversations surrounding patient-centered care USA and long-term healthcare improvement.
This article explores how Dr. Rodolfo Gari’s approach aligns with evolving healthcare priorities and examines the role of innovation collaboration and patient-focused treatment strategies in today’s medical environment.
The Growing Importance of Patient-Centered Care USA
Healthcare systems throughout the country continue shifting toward more personalized models of care.
Traditional healthcare often focused primarily on diagnosis and treatment. While clinical outcomes remain critical modern healthcare increasingly recognizes the importance of communication education accessibility and patient engagement.
The concept of patient-centered care USA focuses on creating healthcare experiences that prioritize individual needs preferences and long-term wellness goals.
Core principles include:
- Shared decision making
- Personalized treatment planning
- Improved patient communication
- Coordinated care delivery
- Enhanced accessibility
- Long-term health management
These principles help create stronger relationships between healthcare providers and patients while supporting improved satisfaction and clinical outcomes.
Many healthcare organizations are embracing patient care improvement initiatives that foster trust and support seamless continuity of care.
Dr. Rodolfo Gari’s healthcare leadership reflects many of these objectives through efforts focused on expanding specialty care services and improving treatment accessibility.
How Dr. Rodolfo Gari Supports Patient-Centered Care USA?
Throughout his career Dr. Rodolfo Gari has worked across multiple areas of healthcare including anaesthesiology pain management and healthcare operations. His experience provides insight into both clinical and administrative aspects of patient care.
His healthcare philosophy has often emphasized improving access to specialized treatment while supporting physician autonomy and patient engagement.
Several aspects of his work align with patient-centered care USA priorities:
Expanding Access to Specialized Care
Many patients with chronic pain encounter difficulties when trying to access the care they need.
These challenges may include:
- Long wait times
- Limited specialist availability
- Fragmented care coordination
- Delayed treatment access
Dr. Gari helped establish and expand pain management practices focused on improving accessibility for patients requiring specialized care.
Supporting Physician-Patient Relationships
Healthcare outcomes often improve when patients feel heard and involved in treatment decisions.
Strengthening physician-patient relationships has been identified as a key organizational priority by groups associated with Dr. Gari.
By enhancing communication and trust, these efforts reinforce patient care improvement strategies aimed at sustaining long-term engagement.
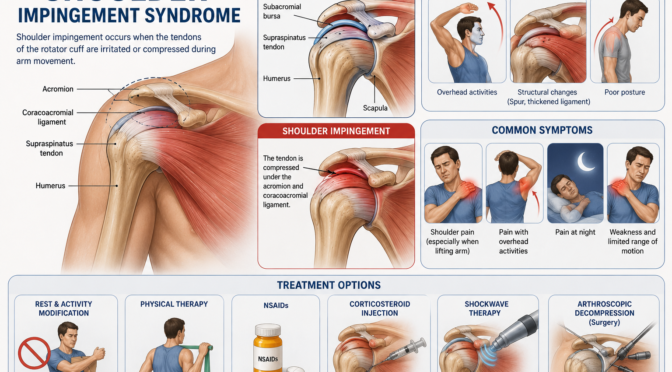
The Role of a Pain Management Specialist USA in Modern Healthcare
Millions of Americans experience chronic pain each year, highlighting its status as a significant and complex healthcare concern.
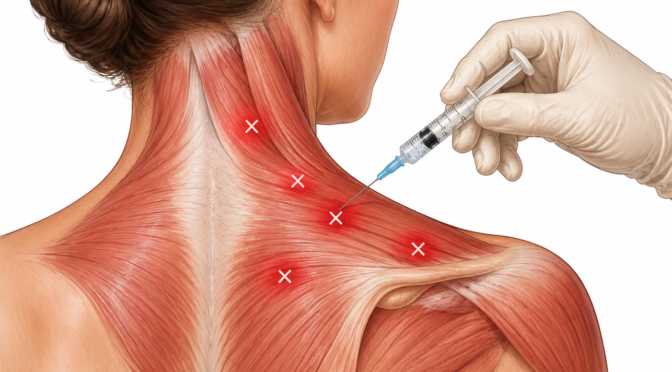
A skilled pain management specialist USA provider plays an important role in helping patients manage conditions that affect mobility function and quality of life.
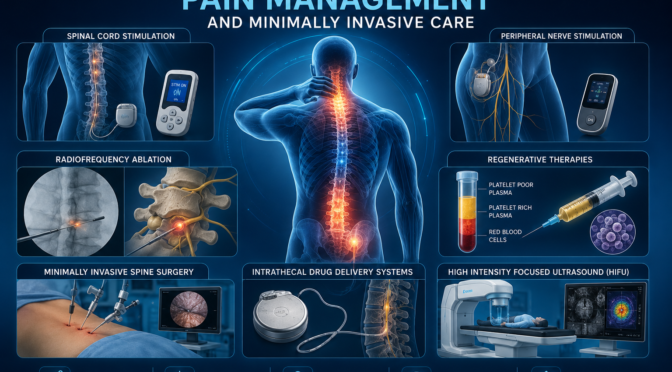
Pain management often requires comprehensive treatment approaches rather than single interventions.
Conditions commonly treated include:
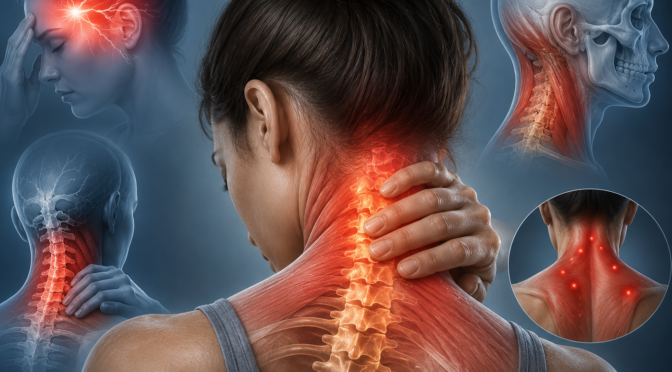
- Back pain
- Neck pain
- Nerve pain
- Joint disorders
- Post-surgical pain
- Chronic musculoskeletal conditions
Dr. Rodolfo Gari’s background includes extensive experience in anaesthesiology and interventional pain management. His work has focused on helping patients access specialized care options designed to improve daily function and symptom management.
Why Pain Management Requires Patient-Focused Care
Pain affects every patient differently.
Successful treatment often requires:
- Individualized assessments
- Ongoing monitoring
- Treatment adjustments
- Multidisciplinary collaboration
This aligns closely with patient-centred care USA principles where treatment plans are designed around individual patient needs rather than standardized approaches.
The role of a pain management specialist USA provider continues growing as healthcare organizations seek more personalized treatment pathways for chronic pain patients.
Patient Care Improvement Strategies Driving Better Outcomes
Healthcare organizations increasingly recognize that improving outcomes requires more than medical expertise alone.
Successful care delivery often depends on operational efficiency communication quality and patient engagement.
Many leading organizations now implement patient care improvement strategies that focus on enhancing every stage of the patient experience.
Examples include:
Improved Communication Systems
Clear communication helps patients better understand:
- Diagnoses
- Treatment options
- Medication instructions
- Follow-up care plans
Patients who feel informed often demonstrate stronger treatment adherence and engagement.
Coordinated Care Models
Fragmented care remains a challenge throughout healthcare.
Integrated care coordination helps ensure:
- Faster referrals
- Better information sharing
- Reduced treatment delays
- Improved continuity of care
These initiatives support broader patient-centered care USA objectives by reducing barriers and improving healthcare navigation.
Data-Driven Quality Improvement
Healthcare leaders increasingly rely on data to evaluate performance.
Organizations may track:
- Patient satisfaction
- Treatment outcomes
- Appointment access
- Care coordination metrics
These patient care improvement strategies help identify opportunities for operational enhancement while supporting long-term quality improvement goals.
Value-Based Healthcare Models and the Future of Care
The healthcare industry continues moving away from volume-focused reimbursement structures toward more outcome-driven systems.
These evolving value-based healthcare models focus on improving patient outcomes while managing costs more effectively.
Rather than rewarding service volume alone healthcare organizations increasingly prioritize:
- Quality outcomes
- Preventive care
- Patient satisfaction
- Care coordination
- Long-term health improvement
This transition aligns naturally with patient-centered care USA initiatives because both approaches emphasize patient well-being rather than transactional care delivery.
How Value-Based Healthcare Models Support Better Outcomes
Value-based care models are most effective when they emphasize preventive care and sustained health outcomes.
Benefits may include:
- Reduced hospital readmissions
- Improved chronic disease management
- Better patient engagement
- Stronger care coordination
Healthcare leaders who embrace these principles help create more sustainable healthcare systems.
Dr. Gari’s focus on integrated specialty care services reflects many goals associated with modern outcome-focused healthcare strategies.
Innovation and Leadership in Patient-Centered Care USA
Healthcare transformation often requires both clinical expertise and organizational leadership.
Over the course of his career Dr. Rodolfo Gari has been involved in developing healthcare organizations focused on specialty treatment access and practice growth.
Healthcare innovation increasingly centres on:
- Expanding patient access
- Improving operational efficiency
- Enhancing treatment personalization
- Supporting interdisciplinary collaboration
These priorities continue shaping the future of patient-centered care USA.
Building Scalable Healthcare Systems
Growing patient demand requires healthcare organizations to develop scalable solutions.
Healthcare leaders often focus on:
- Clinic expansion
- Workforce development
- Technology adoption
- Operational standardization
These efforts help improve access while maintaining care quality.
Supporting Healthcare Professionals
Strong healthcare systems also require physician support.
Many patient care improvement strategies focus not only on patients but also on helping providers spend more time delivering care and less time managing administrative burdens.
Ensuring this balance is essential for the future stability and sustainability of healthcare.
The Future of Patient-Centered Care USA
Healthcare continues evolving rapidly.
Emerging technologies changing patient expectations and new reimbursement models are reshaping how care is delivered.
Future patient-centered care USA initiatives will likely focus on:
- Digital health integration
- Telemedicine expansion
- Personalized treatment planning
- Predictive healthcare analytics
- Enhanced care coordination
At the same time the role of the pain management specialist USA provider will remain important as chronic pain continues affecting large patient populations.
Healthcare organizations implementing advanced patient care improvement strategies and embracing modern value-based healthcare models will be better positioned to meet future healthcare demands.
Leaders who prioritize accessibility communication and personalized treatment will continue influencing positive change throughout the healthcare industry.
Conclusion
The future of healthcare depends on creating systems that place patients at the centre of every decision. Through leadership in pain management healthcare operations and specialty care development Dr. Rodolfo Gari has contributed to broader efforts supporting patient-centred care USA principles. His work reflects the growing emphasis on accessibility physician-patient relationships personalized treatment and long-term healthcare improvement.
By embracing innovative care strategies and value-based approaches, healthcare organizations can deliver more seamless and patient-centered care experiences. If you are seeking specialized treatment and a patient-focused approach to healthcare, consider scheduling a consultation with a qualified provider to explore personalized care options that support your long-term health goals.