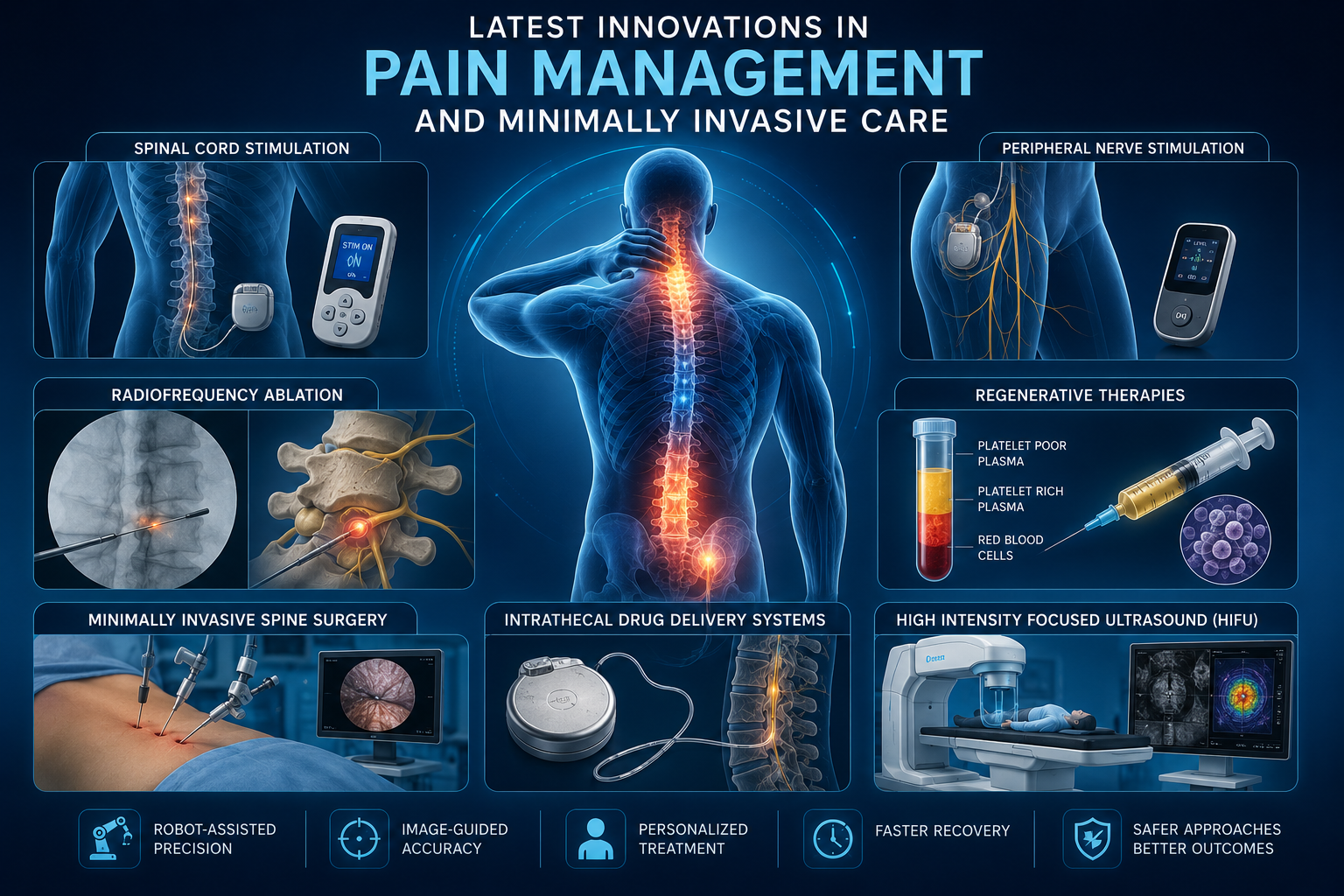
Living with ongoing discomfort can slowly affect every part of your daily routine. From reduced mobility to constant fatigue pain can limit productivity and lower your overall quality of life. This is why pain management innovations have become such an important focus in modern medicine. These new approaches are designed to treat pain at its source while improving comfort and recovery outcomes for patients.
Have you ever tried multiple treatments yet still struggled to find lasting relief? Many traditional methods only address symptoms instead of the underlying cause. This is where advanced pain treatment methods are changing the landscape of care. Instead of relying on temporary fixes modern techniques combine technology precision and personalized strategies to deliver better results.
Over the past decade healthcare providers have embraced minimally invasive solutions that reduce recovery time while improving effectiveness. These pain management innovations are helping patients return to their normal routines faster with fewer complications. They are also reducing the need for long term medication use which is a major concern for many individuals.
In this article you will gain a deeper understanding of how pain management innovations are transforming healthcare. You will also explore how advanced pain treatment techniques work what options are available and how to choose the right approach for your needs.
Understanding Pain Management Innovations and Their Growing Importance
What Defines Pain Management Innovations?
At its core pain management innovations refer to modern medical advancements that improve how pain is diagnosed treated and managed. These innovations focus on delivering targeted solutions that reduce discomfort while supporting long term healing.
Unlike older methods that often relied heavily on medication today’s strategies prioritize accuracy and patient specific care. This shift allows providers to use advanced pain treatment techniques that are more effective and sustainable.
Modern approaches are built on three key principles:
- Precision in diagnosis to identify the exact source of pain
- Targeted therapies that address specific tissues or nerves
- Minimally invasive methods that reduce physical stress on the body
These principles ensure that pain management innovations deliver both immediate relief and long-lasting benefits.
Why Pain Care Is Rapidly Evolving?
The demand for better pain care continues to rise due to increasing cases of chronic conditions. Lifestyle factors repetitive strain and aging populations all contribute to the need for improved solutions.
Another major driver is the growing awareness of the risks associated with long term medication use. This has pushed healthcare providers to adopt advanced pain treatment options that reduce dependence on drugs.
Advances in technology have also been instrumental. Improved imaging tools data analysis and medical devices have made pain management innovations more accurate and accessible than ever before.
The Shift Toward Patient Centred Care
Today’s healthcare systems focus on personalized treatment plans. This means that each patient receives care tailored to their specific condition and lifestyle.
With the help of pain management innovations providers can now:
- Assess pain patterns more effectively
- Customize treatment strategies
- Monitor progress in real time
This personalized approach is a defining feature of modern advanced pain treatment.
Breakthrough Technologies Driving Pain Management Innovations
Image Guided Precision Treatments
One of the most impactful developments in pain management innovations is the use of advanced imaging technologies. Tools such as ultrasound and fluoroscopy allow providers to see inside the body in real time.
This level of precision ensures that treatments are delivered exactly where they are needed. It also reduces the risk of complications and improves outcomes.
Benefits of image guided techniques include:
- Greater accuracy in targeting pain sources
- Reduced procedure time
- Improved patient safety
These advantages make imaging a cornerstone of advanced pain treatment.
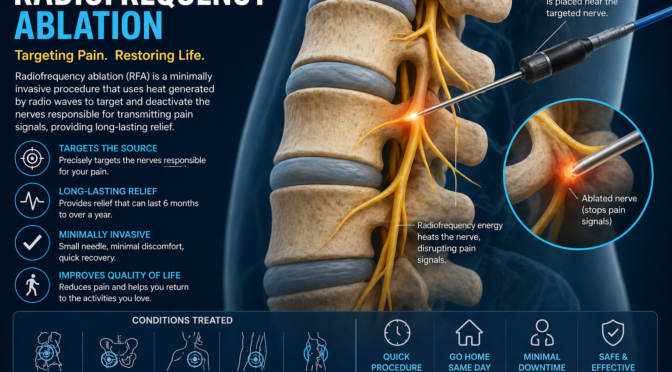
Radiofrequency Ablation for Long Term Relief
Radiofrequency ablation is a modern technique that uses controlled heat to interrupt pain signals from nerves. It is widely used in pain management innovations for conditions such as chronic back pain.
Patients often experience relief that lasts for months or even longer. This makes it an excellent option for those seeking durable results.
Key benefits include:
- Long lasting pain relief
- Minimal downtime
- Reduced need for repeated treatments
This approach represents a major step forward in advanced pain treatment.
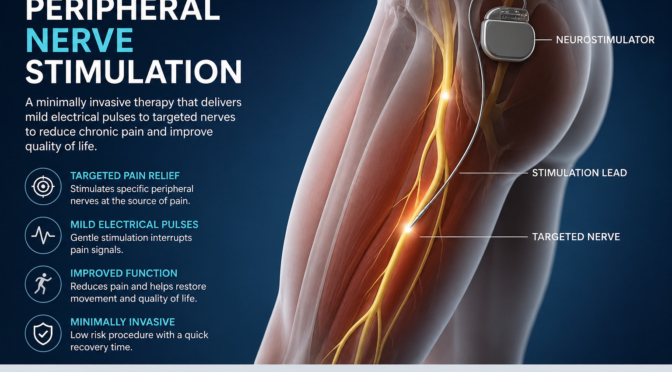
Neuromodulation and Electrical Therapies
Neuromodulation involves altering nerve activity using electrical stimulation. Devices such as spinal cord stimulators are commonly used in pain management innovations.
These systems send signals that block pain messages before they reach the brain. Patients can often adjust the settings to suit their comfort levels.
Advantages include:
- Customizable pain control
- Reversible treatment option
- Improved daily functioning
Neuromodulation continues to expand the possibilities of advanced pain treatment.
Regenerative Medicine in Advanced Pain Treatment
Platelet Rich Plasma Therapy
Platelet rich plasma therapy is a natural approach that uses components from the patient’s own blood to promote healing. It is a key part of pain management innovations focused on tissue repair.
This therapy works by delivering growth factors directly to damaged areas. These factors stimulate the body’s natural healing processes.
Benefits include:
- Faster tissue recovery
- Reduced inflammation
- Lower risk of adverse reactions
PRP is widely used in advanced pain treatment for joint injuries and muscle conditions.
Stem Cell Based Therapies
Stem cell therapy is another breakthrough in pain management innovations. These cells can develop into different types of tissue which makes them ideal for repairing damage.
This approach is especially useful for conditions that involve degeneration such as arthritis.
Key advantages include:
- Long term healing potential
- Improved joint function
- Reduced pain levels
Stem cell therapy represents a powerful advancement in advanced pain treatment.
The Future of Natural Healing Approaches
Regenerative medicine is gaining popularity because it addresses the root cause of pain. Instead of masking symptoms these therapies aim to restore normal function.
Patients are increasingly choosing pain management innovations that support natural healing. This trend highlights the growing importance of advanced pain treatment in modern healthcare.
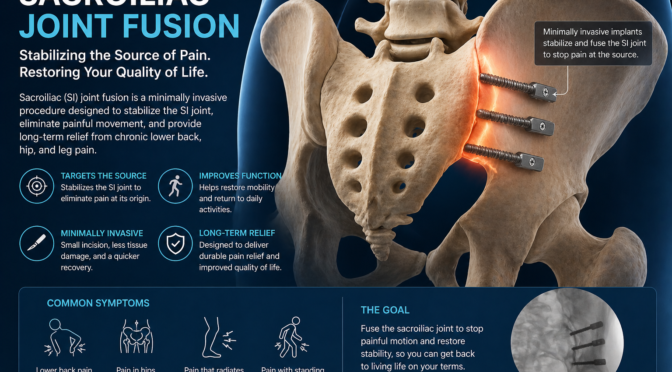
Minimally Invasive Procedures Transforming Pain Care
Epidural Steroid Injections
Epidural injections are commonly used in pain management innovations to treat spinal conditions. These injections deliver anti-inflammatory medication directly to affected nerves.
Patients often experience rapid relief along with improved mobility.
Benefits include:
- Reduced inflammation
- Quick recovery
- Targeted pain relief
These injections are a key component of advanced pain treatment strategies.
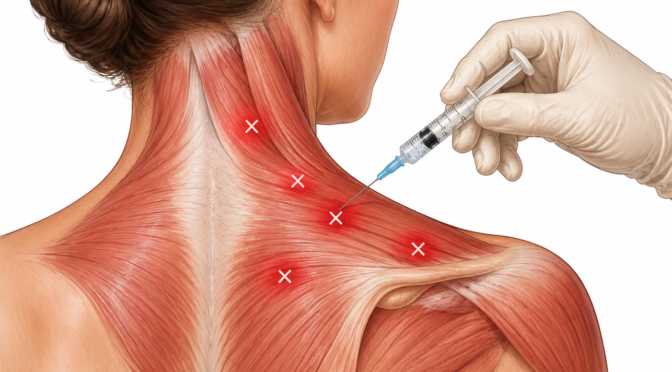
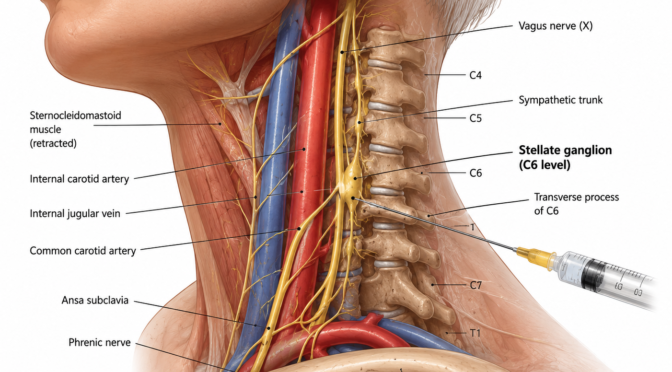
Nerve Blocks for Precise Relief
Nerve blocks involve injecting medication near specific nerves to stop pain signals. This technique is widely used in pain management innovations.
It is effective for both diagnosis and treatment of various conditions.
Advantages include:
- Immediate pain reduction
- High precision
- Minimal discomfort during the procedure
Nerve blocks are an essential part of advanced pain treatment.
Why Is Minimally Invasive Care Preferred?
Minimally invasive procedures are becoming the standard in pain management innovations because they reduce risk and recovery time.
Patients benefit from:
- Smaller incisions
- Less tissue damage
- Faster return to normal activities
These factors make minimally invasive methods a cornerstone of advanced pain treatment.
Digital Health and Its Role in Pain Management Innovations
Telemedicine Expanding Access to Care
Telemedicine has transformed how patients receive care. It allows individuals to consult with specialists from the comfort of their homes.
This is especially valuable for those with mobility issues or limited access to healthcare facilities.
Benefits include:
- Convenient consultations
- Reduced travel time
- Continuous follow up care
Telemedicine supports the growth of pain management innovations.
Wearable Devices for Monitoring Pain
Wearable technology provides real time data on physical activity and pain levels. These devices are becoming an important part of advanced pain treatment.
They help providers track progress and adjust treatment plans accordingly.
Advantages include:
- Personalized insights
- Better treatment outcomes
- Increased patient engagement
Wearables are shaping the future of pain management innovations.
Artificial Intelligence in Treatment Planning
Artificial intelligence is enhancing pain management innovations by analyzing large amounts of patient data. This helps providers make more accurate decisions.
AI driven systems can:
- Predict treatment outcomes
- Identify patterns in pain behaviour
- Optimize care plans
This technology is revolutionizing advanced pain treatment.
Benefits of Advanced Pain Treatment for Patients
Enhanced Quality of Life
One of the most important outcomes of pain management innovations is improved quality of life. Patients can return to their daily activities with greater comfort.
Reduced Dependence on Medication
Modern advanced pain treatment methods reduce the need for long term medication use. This lowers the risk of side effects and improves overall health.
Faster Recovery Times
Patients benefit from shorter recovery periods thanks to minimally invasive procedures. This allows them to resume normal activities more quickly.
Personalized Care for Better Results
Pain management innovations focus on individualized treatment plans. This ensures that each patient receives the most effective care possible.
Choosing the Right Pain Management Approach
Evaluating Your Condition
Selecting the right treatment begins with understanding your specific condition. Factors such as pain severity and duration play a key role.
Consulting a Specialist
A qualified provider can guide you through available pain management innovations and recommend the best options for your needs.
Combining Treatments for Optimal Outcomes
In many cases combining multiple therapies provides better results. This integrated approach is a key feature of advanced pain treatment.
Conclusion: Embracing Pain Management Innovations for Better Health
The evolution of healthcare has brought remarkable progress in how pain is treated and managed. Pain management innovations now offer safer more precise and highly effective solutions for individuals dealing with chronic or acute discomfort. These modern approaches focus on long term relief while improving overall well-being.
If you are looking for a better way to manage pain exploring advanced pain treatment options can make a meaningful difference. With the right care plan, you can regain mobility reduce discomfort and improve your quality of life. Book your consultation today and take the first step toward lasting relief with pain management innovations.